
In general, the advantages and disadvantages of the different rapid antigen tests technologies indicate that the most suitable technology should be determined by the testing strategy’s goals, not the other way around. In practice, testing has three primary objectives:
- Accurate diagnosis of patients to inform clinical care decisions.
- Confirming or disconfirming suspected cases, e.g. due to the presence of symptoms or contact with a confirmed case, to inform TTTI strategies.
- Monitoring specific population groups where infections are suspected to occur (e.g. nursing homes, companies, schools and universities, geographic areas with suspected clusters, etc.).
None of the presently available testing methods are suited for all three situations, and the varying prices and logistical needs must be considered when determining which rapid antigen tests to employ for what and on whom. In each of the three cases. Additionally, testing technologies may be coupled to accomplish testing strategies’ goals, and tests can be repeated to adjust for poorer testing accuracy. For example, as discussed below, RT-PCR may be used to validate questionable rapid antigen tests findings, and repeated rapid antigen tests improve the likelihood that their results are correct. learn more about rapid antigen tests by clicking here.
While point-of-care RT-LAMP and CRISPR-based testing have the potential to solve some of the constraints associated with RT PCR and rapid antigen tests, their development is continuing, and they are not yet commercially accessible. Additionally, the practical ramifications of administering these rapid antigen tests are unknown at the moment.
Diagnosis of patients to aid with clinical decision-making
Due to their increased sensitivity and specificity, RT-PCR testing (and comparable molecular rapid antigen tests) remain the gold standard in this setting. In the long future, point-of-care RT-LAMP and CRISPR-based diagnostics may serve as a supplement to RT-PCR due to their high reproducibility. The purpose in the clinical context is to minimize the possibility of misdiagnosis and inappropriate care, which may have major unfavorable implications for patients. This is especially critical during the winter when many respiratory infections are circulating. As a result, the most trustworthy test will always be preferred.
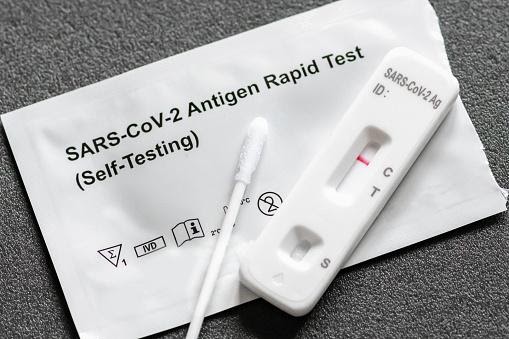
By validating suspected and contact cases, use in testing, tracking, tracing, and isolating
This scenario entails confirming or disconfirming infection in individuals who present with symptoms in an outpatient environment (as a first diagnostic step) and in those who have been in touch with a confirmed case to guide TTTI measures. RT-PCR rapid antigen tests (and comparable molecular tests) are equally suited for this purpose and will continue to be the gold standard in such settings for the foreseeable future. However, cost and capacity limits may limit their applicability for verifying suspected cases, particularly in large numbers. Rapid antigen tests at the point of care may be utilized in this situation if RT-PCR cannot be employed.
The benefit of point-of-care rapid antigen tests in TTTI techniques stems from their enhanced speed and cost savings, which may compensate for their lower sensitivity. Rapid antigen test models (HAS, 2020[9]) propose that:
• Reduced sensitivity may be compensated for by doing a greater number of rapid antigen tests. However, with a sensitivity of 70%, the number of rapid antigen tests must be increased by at least 50%.
• Reduced sensitivity may be compensated for by obtaining data more quickly. The effect of this time gain is obviously dependent on the point in time at which the person is tested following the onset of symptoms (the closer to the onset, the greater the impact), but receiving a result instantly (as opposed to two days after taking the test) may reduce the possibility of transmissions by approximately 30%. This suggests that the primary usefulness of these rapid antigen tests may be to deliver data more rapidly and facilitate isolation in symptomatic individuals immediately after symptom onset.
In summary, if RT-PCR findings cannot be obtained within 24 to 48 hours or the number of individuals to be tested exceeds the capacity of RT-PCR, point-of-care rapid antigen tests may be utilized as a second-best choice for rapid diagnosis of symptomatic and asymptomatic patients in outpatient settings. Given the broad range of sensitivity of presently available rapid antigen tests, it is critical to choose the most sensitive antigen testing.
Observation of certain demographic groupings
Early identification of clusters in certain subpopulations will be critical when existing containment and mitigation measures, including a second wave of general population lockdowns in certain nations, begin to be released. This may help avoid the need for another round of expensive containment measures until a vaccine is ready in sufficient numbers.
For monitoring particular populations such as nursing homes, universities, schools, and businesses, or any demographic where a new cluster of illnesses is expected to emerge, point-of-care rapid antigen tests are the most suitable technique but may need recurrent testing. To begin, this is because new infections may arise at any moment, resulting in the random formation of new clusters, necessitating constant testing to enhance the likelihood of identifying them. Second, regularly repeating rapid antigen tests enhances testing accuracy.
However, it is important to keep in mind that good findings acquired in these situations may still need confirmation using RT-PCR. When prevalence is low, a high rate of false positives might be a serious issue.
For certain applications, wastewater surveillance may be utilized to monitor huge population groups in particular locations. It has now been shown conclusively that individuals infected with COVID 19 shed virus in their faeces, even before symptoms emerge. Wastewater-based monitoring of nursing homes, businesses, schools, and specific neighborhoods, for example, might identify the emergence and volatility of COVID 19, perhaps providing actionable information to advise “reopening” or to commence more thorough testing.
Testing to ensure the safety of air travel
Rapid antigen tests are increasingly being used in conjunction with air travel to guarantee that only those who test negative are permitted to fly and to waive or ease quarantine restrictions upon arrival. It should be emphasized, however, that air travel may increase exposure to the virus due to the difficulty of implementing physical distancing measures. Taking a trip entails spending time in congested airport facilities such as security and boarding lines, as well as many hours in the confined space of an aircraft with other passengers, particularly on long-haul flights.
Additionally, it may include commuting to and from airports through public transportation. While testing may assist in mitigating risk, it cannot completely remove it. Testing must thus be used in conjunction with other preventive steps taken before to, during, and after travel to minimize the risk of travelers spreading the virus. This also implies that the practicalities of implementing a dependable air travel testing plan might be complicated.
